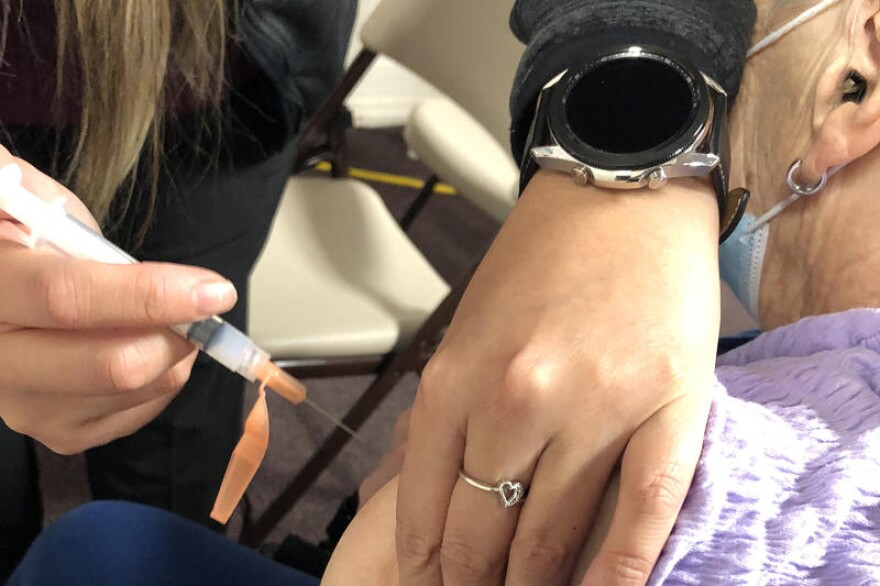
The demand for COVID-19 vaccines in Indiana is slowing down, even as the state hits 2 million fully vaccinated Hoosiers. And some experts are concerned that vaccine hesitancy may prevent us from reaching herd immunity. But hesitancy is more complicated than just distrust.
Dr. Michael Weiner is a Regenstrief Institute scientist and Indiana University professor of medicine. He said vaccine hesitancy or reluctance falls into three broader categories: convenience, confidence and complacency.
Convenience refers to eligibility and access. Confidence is the trust – or lack thereof – in vaccine safety. And complacency describes populations who already feel protected enough.
While convenience has been improved since Indiana opened eligibility to all Hoosiers 16 and older – and asked state-run sites to accept walk-ins – confidence and complacency are more in the spotlight.
"There’s probably still some increased reluctance among younger groups that may view themselves as less at risk or view the vaccine as less important for them," he said.
Weiner said it makes sense that older Hoosiers are more likely to have received vaccines than younger Hoosiers because they've had access longer. But age and race remain the biggest indicators of whether or not someone has likely gotten at least one dose of vaccine – with Black and Latinx communities farther behind.
Different groups fall into these different aspects of vaccine hesitancy, but Weiner said – in some cases – religion, politics and geography create barriers to vaccination.
And vaccine hesitancy – convenience, confidence or complacency – is a barrier to achieving herd immunity.
Weiner said, first, it’s important to remember that herd immunity does not mean eradication of COVID-19, but it is a tool to help get there.
READ MORE: How Will Indiana Distribute COVID-19 Vaccines? Here's What You Need To Know
Join the conversation and sign up for the Indiana Two-Way. Text "Indiana" to 73224. Your comments and questions in response to our weekly text help us find the answers you need on COVID-19 and other statewide issues.
Indiana’s more than 725,000 confirmed COVID-19 cases also contribute to herd immunity.
"We would expect that most of the herd immunity would be attributable to vaccinations – a significant amount from the infections, but not the majority," Weiner said.
State health officials have not set a benchmark for herd immunity. There isn’t really a hard and fast rule, though many experts nationwide point at 75 percent to 85 percent inoculated as the threshold for COVID-19.
Contact Lauren at lchapman@wfyi.org or follow her on Twitter at @laurenechapman_.