Union County is small — only one Indiana county has fewer people. A block away from the courthouse in Liberty, a small building pulls double duty as the health department and area planning office.
Here, a young woman in pajamas is sitting with her head in her arms. She’s here to be assessed for a new medical device that might give her almost instant relief from her painful drug withdrawal symptoms.
Jeff Mathews is co-manager of the Union County Opiate Treatment Center (he’s also the area planning director). He’s in charge of the Liberty-based pilot program for the new medical device, called the “Neuro-Stim System Bridge.” It’s a gadget, worn outside the ear that uses electric signals to relieve opioid withdrawal symptoms.
“It’s not the fix,” says Mathews of the device. “[But] it’s a tool that I can put on someone that will relieve the symptoms for them to get them to the part where they’re clean.”
Indiana is one of the many states that has been wrestling with how to decrease its residents’ drug use — especially of opioids, a class of drugs that includes heroin and some prescription painkillers. The Indiana State Department of Health estimates almost 600 people died from opioid overdoses last year.
When a person who’s been using opioids abruptly stops, withdrawal can be so unbearable a person relapses to get relief. Withdrawal symptoms, says Mathews, are often described as “the worst flu you’ve ever had times a thousand.”
“Shaking knees, convulsions, throwing up, diarrhea,” he says. “I mean, you’re sick.”
For years, those symptoms proved too much for Tom, a landscape worker in Union County. He became addicted to prescription painkillers after a bout of knee surgeries. We're not using his last name to protect his anonymity.
“Once you get to day two or three, if you’ve got a family or a job and you’re trying to function, you can’t,” Tom explains. “So your only option is, boom, I got these, I can get by.”
A few months ago, he learned about the bridge pilot through Mathews, a friend. He wore it for five days and was able to get through that crucial, first week. Tom says the effects of the bridge were immediate.
“Literally within ten or 15 minutes my stomach was growling—you can’t eat when you’re going through the withdrawals,” Tom says. “I wasn’t thinking about being in the withdrawal, I mean I actually felt like, ‘I’m going to work.’”
And he did. After he put the bridge on, he went to work and put in a whole day.
Like Tom, every one of the patients in this pilot - dozens of people - have used the device to get through withdrawal and into medication-assisted treatment.
It is made by Indiana-based Innovative Health Solutions, which supplies the pilot’s devices for free – paying it forward for wider distribution in the future.
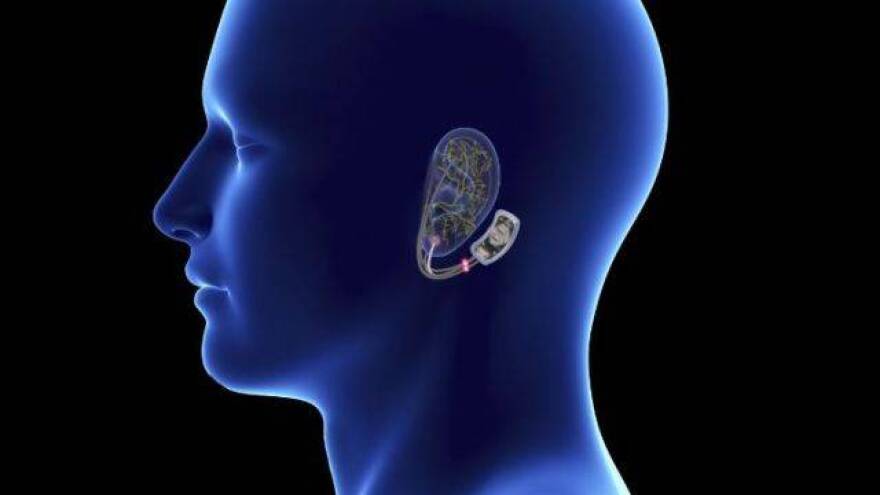
Here’s how it works: the bridge is flat, made of plastic and is about the size of a quarter. It sticks to a person’s head with adhesive. Thin wires come out of the bridge and are shallowly implanted in the skin around the ear. Tiny electric pulses travel through the wires down the nerves to parts of the brain that control pain and change the sensation, reducing a person’s perception of discomfort.
After five days, the bridge is taken off and thrown away—the batteries won’t recharge. Then, the person is ushered into counseling and other medication.
Even though the bridge is FDA-cleared, research is still being conducted. Xioake Chen, a Stanford professor who researches withdrawal pain and the brain, says the idea is interesting, but he’d like to see more evidence.
“For this kind of research to be accepted by broad audiences, you need to go through the peer-reviewed publication process,” Chen says.
Chen says electrodes have been used to treat neurological symptoms before, but they’ve been implanted deep in the brain in well-known locations. The bridge is worn on the outside, so Chen says it would be a challenge to selectively modulate the right places without side effects.
Another hurdle? Cost. The bridge costs nearly $500 per device, and insurance doesn’t cover it (though Mathews says he’s confident that could change).
There’s no telling when it might become more widely available, though Union County’s pilot is open to everyone. Local residents get priority, but patients from other counties and states have participated.
Mathews is optimistic, but he underlines adamant the new treatment only gets a person through withdrawals.
“It’s not like at the six-month point they’re no longer addicts, or at the year point or at the five-year point,” he says. “They’re always going to have that addition.”
But the bridge is promising that a small piece of the recovery has just been made easier.